Fungal Infection (Tinea)
Skin Treatments
Other Treatments
Have Any Question?
Request a Call Back
What is Dermatophyte infection?
Dermatophyte infection is a superficial fungal infection of skin, hair and nails. It is also known as ringworm. In Hindi it is termed as Daad and in Marathi it is termed as Gachkaran.
How can one get a Dermatophyte Infection?
Ringworm occurs when a person gets infected with Dermatophytes which is a superficial fungus. This fungus lives off human keratin and that is why the infection can occur on the skin, hair and nails.
How does the infection spread? What are the predisposing factors for the development of Dermatophyte infection?
Dermatophyte infection is transmitted by direct skin contact with infected person and by sharing objects of daily use (fomites).
- Dermatophyte infection is more common in tropical climate.
- High temperature, humidity and occlusive atmosphere predisposes to development of Dermatophilosis
- Certain diseases like diabetes mellitus, HIV infection or patients taking steroids or anticancer drugs are high risk for development of Dermatophilosis.
- Poor hygiene, increased sweating, self- medication or use of topical steroids, steroid- antifungal combinations, infection in family members are contributory factors.
How does Dermatophyte infection appear? Which areas of the body are affected?
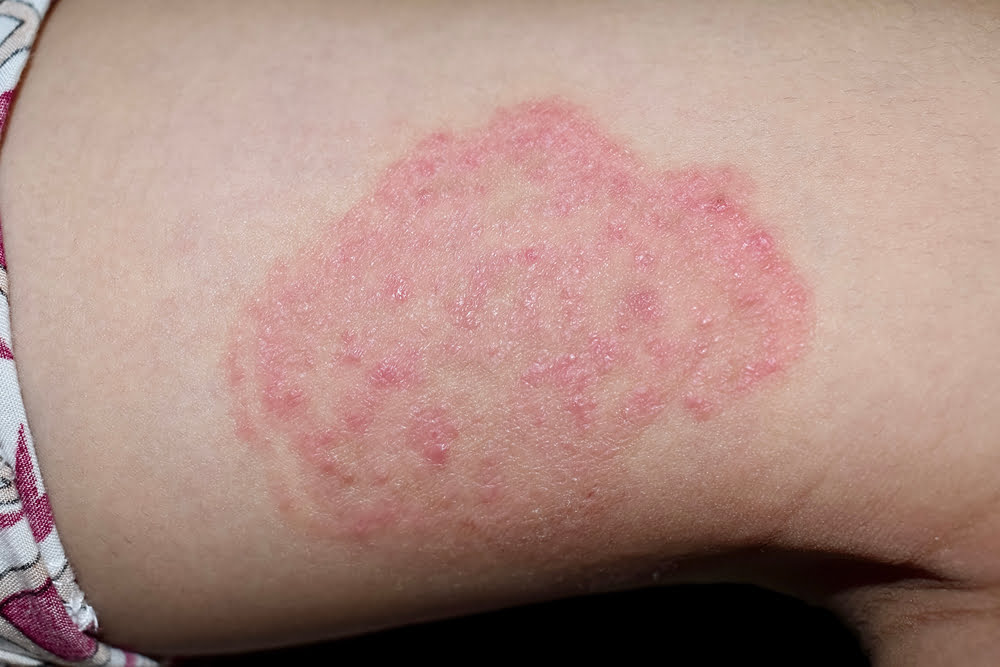
- Dermatophyte infection presents with severe itching and skin lesions in the form of circular red areas with raised border and central clearing. The infection clears in the centre and extends towards the periphery.
The folds of the body are the most common sites affected, especially the groins (hence termed jock itch), the armpits, areas below the breasts. The infection can extend onto the abdomen, buttocks and thighs.
The palms, soles, web spaces of fingers and toes may present with itchy and scaly lesions.
Nails may be infected and act as a source for recurrent Dermatophytosis. The nails may show discoloration or total damage of the nail plate can be seen. Toe nail infections are common in elderly and diabetic patients.
Hair infection and appears as scaly patches with loss of hair or severe infections with pus filled lesions may be seen. Hair involvement is common in children.
What should one do if he/she gets Dermatophyte infection?
Consult a dermatologist since it can be easily diagnosed by the presence of itching clinical appearance of the lesions.
Are there any laboratory tests to diagnose Dermatophytoses?
Diagnosis is usually done by dermatologist based on clinical features. If needed, scrapings from the skin or clippings of the nail and hair can be subjected to laboratory tests to confirm the diagnosis and identify the causative fungus by microscopy and culture.

